
It seems like everyone these days has heard of gluten, along with The Top 5 Reasons Gluten Will Make You Dumber, The #1 Reason Why Your Dog Should Go Gluten Free, and Give Up Gluten – Live to 150. I’m joking of course…but in the clamor of misinformation about gluten, it’s easy to lose sight of the fact that gluten is a serious problem for millions of people. I’m talking about the 1% of the world’s population who have celiac disease, one of the most under-diagnosed disorders around.
Since May is Celiac Awareness Month, I’d like to take the time to revisit the basics: What celiac disease is, how it is diagnosed and treated, and where to get more information.
What is Celiac Disease?
Celiac disease is a hereditary autoimmune intestinal disorder that affects both children and adults. It can develop at any age. When an individual with this disorder consumes gluten (proteins found in the grains wheat, barley and rye), an immune reaction is triggered in the small intestine.
Tiny finger-like projections or villi in the small intestine become inflamed and eventually damaged from continued exposure to gluten. This process, called “villous atrophy,” may occur rapidly or gradually over time. As a result, the body is unable to adequately absorb nutrients, especially iron, calcium, vitamin D and folic acid. Also, malabsorption of carbohydrates (e.g., lactose [the carbohydrate in milk]), protein and other nutrients may occur.
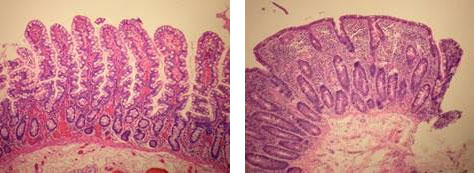
Untreated celiac disease can lead to (1) nutrition-related deficiency conditions such as anemia and osteoporosis, (2) neurological complications, (3) infertility in both women and men, (4) an increased risk of miscarriage or of having a low-birth-weight baby, and (5) an increased risk of certain types of cancers.
Prevalence of Celiac Disease
Originally thought to be a rare disorder, celiac disease is now recognized as one of the most common inherited diseases. Serological (blood) screening tests have revealed that the global prevalence is approximately 1% of the population, although in some countries (e.g., Finland and Sweden) the rate is as high as 2%–3%. Celiac disease is common in people of North American and European ancestry, as well as in the populations of South America, North Africa, India, Pakistan and the Middle East.
Symptoms and Presentations of Celiac Disease
Celiac disease affects not only the gastrointestinal tract but also many other organ systems in the body. Below are some of the many symptoms that can vary in severity from one person to another. Onset of symptoms may appear suddenly or gradually, and may progress slowly or rapidly. Some individuals have “silent celiac disease”, displaying no or very subtle symptoms in spite of the presence of villous atrophy. For many adults, one of the most common presentation is iron-deficiency anemia.

- Abdominal pain, bloating and gas
- Indigestion/reflux (“heartburn”)
- Nausea and vomiting
- Ongoing or intermittent diarrhea and/or constipation
- Lactose intolerance
- Chronic fatigue and weakness
- Iron, folic acid and/or vitamin B12 deficiencies
- Other vitamin and mineral deficiencies (e.g., A, D, E, K, calcium, zinc)
- Weight loss (note that CD also can occur in overweight or obese individuals)
- Bone/joint pain
- Bone disease (osteomalacia, osteopenia, osteoporosis)
- Muscle cramps
- Easy bruising of the skin
- Itchy, blistering rash (dermatitis herpetiformis)
- Tingling or numbness in hands and feet (peripheral neuropathy)
- Swelling (edema) of hands and feet
- Migraine headaches
- Seizures
- Mood swings
- Depression
- Elevated liver enzymes
- Mouth ulcers (canker sores)
- Menstrual irregularities
- Infertility (in women and men)
- Recurrent miscarriages
Additional symptoms of celiac disease in children
- Failure to thrive (delayed growth and short stature)
- Irritability and behavioral changes
- Concentration and learning difficulties
- Delayed puberty
- Dental enamel abnormalities (discoloration, loss of tooth enamel)
Diagnosis of celiac disease
Diagnosis of celiac disease often is very difficult because of its diverse range of symptoms, some of which overlap with other conditions. Many individuals with celiac disease are misdiagnosed as having other disorders such as irritable bowel syndrome (IBS), lactose intolerance, ulcers and/or chronic fatigue syndrome. It has been shown that individuals with celiac disease see multiple physicians over an average of 11 years before receiving a definitive diagnosis, as shown in research studies conducted at Columbia University in New York and by the Canadian Celiac Association. Other countries have reported similar delayed diagnosis rates. It is estimated that 60-70% of individuals with celiac disease still remain undiagnosed.
Because it is a genetic condition, all first-degree relatives (parents, siblings, children) of celiac individuals should be screened for the disease. First-degree relatives have a 5-15% risk of developing celiac disease at any age. However, a negative screening test result does not rule out the possibility that a family member could develop the disease in the future. Therefore, if a family member subsequently experiences celiac-related symptoms in spite of previous negative celiac serology results, repeat testing is recommended.
Various blood tests are used to screen for celiac disease including:
- IgA and IgG tissue transglutaminase (tTG)
- IgA endomysial (EMA)
- IgA and IgG deamidated gliadin peptide (DGP) antibody tests
Small intestinal biopsy in celiac diagnosis
The definitive test for diagnosing celiac disease is a small intestinal biopsy, done in a hospital or clinic endoscopy unit.
A gluten-free diet should never be started before the celiac blood and small intestinal biopsy tests are completed, as this can interfere with making an accurate diagnosis.
Treatment of celiac disease

Currently, the only treatment for celiac disease is a strict gluten–free diet for life. Following the diet will result in improved health and well-being, as well as greatly reduce the risk of celiac-related complications. The time needed for resolution of symptoms and the healing process varies considerably, with children tending to heal more quickly and completely than adults. Individuals with long-standing untreated celiac disease may require several years on the diet before the small intestinal damage is repaired. In some cases complete healing may not occur, especially if the villous atrophy is severe and/or in older adults with long-standing symptoms prior to diagnosis.
Due to the complexities of the gluten-free diet, consultation with an expert registered dietitian (RD) is highly recommended. After completing a thorough nutritional assessment, s/he will address any nutritional concerns and will work with the individual to learn how to successfully adapt to the gluten-free lifestyle. Practical information about label reading, meal planning, shopping, budgeting, food preparation, cross-contamination and eating away from home will be provided, as well as suggestions on how to effectively cope with the social and emotional aspects of following the diet. Joining a celiac group for further information and ongoing support also is beneficial (see below).
Dermatitis Herpetiformis
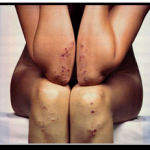
Dermatitis herpetiformis (DH) is another presentation of celiac disease. This chronic skin condition is characterized by an intense itchy and blistering rash. The rash is symmetrically distributed on both sides of the body. Commonly found on the elbows, knees and buttocks, it also can occur on the back of the neck, upper back, scalp and hairline. Initially, groups of small blisters (looking similar to those of chicken pox or herpes) are formed on the skin, and these soon erupt into small erosions. Most people with DH have varying degrees of small intestinal villous atrophy, although some have no gastrointestinal complaints.
Diagnosis of dermatitis herpetiformis
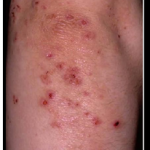
Individuals with DH frequently are misdiagnosed as having other skin conditions such as eczema, contact dermatitis, allergies, hives, herpes or psoriasis. The only way to correctly diagnose DH is with a skin biopsy from unaffected skin adjacent to blisters or erosions. A small intestinal biopsy is not required if the skin biopsy is positive for DH.
Treatment of dermatitis herpetiformis
The treatment for DH is a strict gluten–free diet for life. Following the diet allows the gastrointestinal damage to resolve within several months and over time results in an improvement in the skin lesions. Depending on the severity of the rash, between six months to two years on the diet may be necessary in order for the skin to heal completely.
Celiac Disease Resources
Check out the following resources for more information about celiac disease and the gluten-free diet:
American Celiac Organizations
Canadian Celiac Organizations
 Ready to learn more? Check out my latest edition of Gluten-Free: The Definitive Resource Guide – Revised Edition. It covers all aspects of nutrition and the gluten-free diet, while offering healthy eating guidelines, meal plans, recipes, detailed information about safe foods/ingredients and labeling, helpful resources and more. Get it here!
Ready to learn more? Check out my latest edition of Gluten-Free: The Definitive Resource Guide – Revised Edition. It covers all aspects of nutrition and the gluten-free diet, while offering healthy eating guidelines, meal plans, recipes, detailed information about safe foods/ingredients and labeling, helpful resources and more. Get it here!
